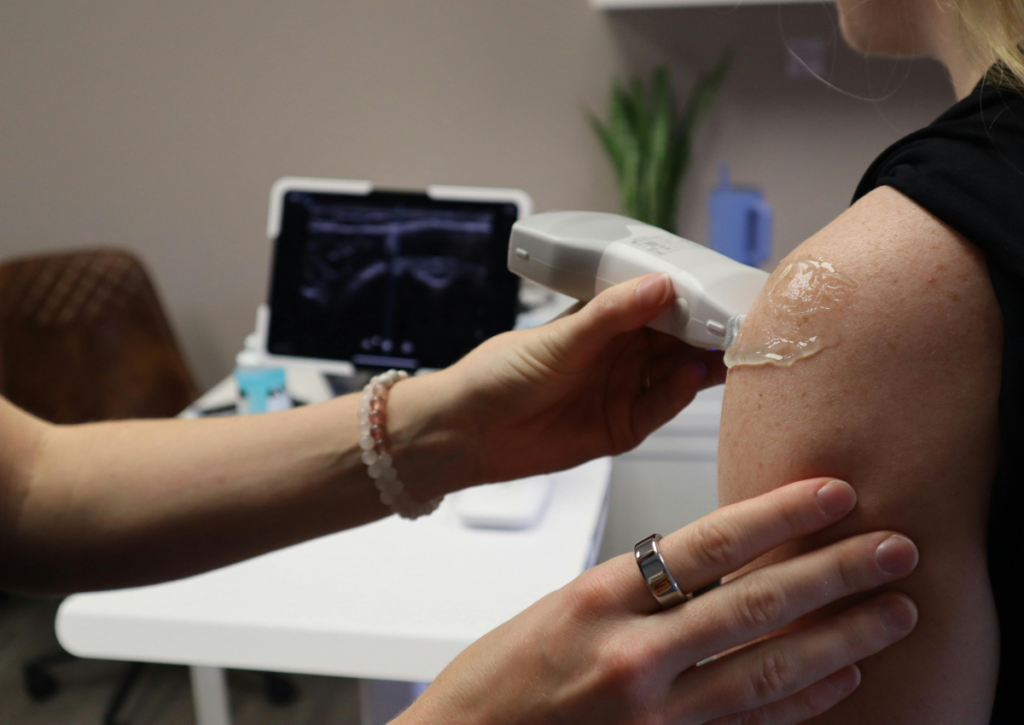
It starts small. A twinge when you reach for something on a high shelf. A dull ache that wakes you up when you roll onto your shoulder at night. You ignore it for a week, maybe two. Then one morning, you try to comb your hair and realize your arm will not go up. Hooking your bra, tucking in your shirt, reaching for your wallet in your back pocket – suddenly, these tiny everyday movements feel impossible.
Welcome to frozen shoulder. And if you are living in Indore, chances are higher than you think that this condition will knock on your door – especially if you are over 40, diabetic, or have ever had your arm in a sling after an injury.
The medical name is adhesive capsulitis, but patients know it by a simpler description: “My shoulder is stuck and it hurts like nothing else.” The frustrating part? Most people get wrong advice early on. They are told to rest it. They are given painkillers and told it will “settle on its own.” Months pass. The shoulder gets stiffer. The pain gets worse. And by the time they finally reach the right professional, recovery takes twice as long as it should have.
This article is your shortcut. Everything you need to know about frozen shoulder treatment in Indore – what causes it, why it is so common here, and exactly how hands-on physiotherapy gets your arm moving again – is laid out below. No jargon, no fluff, just the facts.
The Indore Problem: Why Frozen Shoulder Is More Common Here Than You Think
India has one of the highest rates of diabetes in the world, and Indore is no exception. According to published research, frozen shoulder affects 10% to 38% of people with diabetes – compared to roughly 2% to 5% of the general population. That is a staggering difference.
Why does diabetes cause frozen shoulder? When blood sugar remains elevated over time, the excess glucose molecules attach themselves to collagen fibers in the shoulder capsule. This process, called glycosylation, makes the capsule tissue thick, sticky, and inflexible. The shoulder literally stiffens from the inside out, and the person may not even connect it to their diabetes.
Indore’s growing diabetic population, combined with a large number of people in the 40 to 60 age group, sedentary work culture, and thyroid disorders (another major risk factor), creates the perfect storm for frozen shoulder. Add to this the local tendency to “wait it out” or rely solely on painkillers, and you get thousands of people living with avoidable shoulder disability for months or even years.
A clinical review published on PubMed confirms that while most frozen shoulder patients respond well to conservative treatment within 12 to 18 months, diabetic patients tend to have more severe disease and take longer to recover. This makes early, skilled physiotherapy even more important for this group.
A Shoulder That Freezes in Three Acts – And Where You Are Right Now
Frozen shoulder does not happen overnight. It follows a remarkably predictable pattern of three stages, and understanding which stage you are in changes everything about how your treatment should be planned.
Act 1: The Freezing Stage (2 to 9 Months)
This is the painful stage. Your shoulder aches constantly – at rest, during movement, and especially at night. Every week, you notice that your arm moves a little less than before. Reaching overhead becomes difficult first. Then reaching behind your back. Then reaching across your body. The pain is sharp during movement and a deep, dull throb at rest.
This is the stage where most people make the critical mistake of resting the shoulder completely. Rest feels logical when something hurts, but in frozen shoulder, stopping movement is the worst thing you can do. The less you move it, the faster the capsule tightens. Gentle, guided movement during this stage can dramatically shorten how long the freezing lasts.
Act 2: The Frozen Stage (4 to 6 Months)
Strangely, the pain actually reduces during this stage. Many people think they are getting better. But the stiffness is now at its peak. Your shoulder is locked in a very limited range. You cannot lift your arm above shoulder height. Dressing, bathing, and driving become daily battles. Work tasks that require any overhead reaching become impossible.
This is the stage where physiotherapy makes its biggest impact. The shoulder capsule has thickened and contracted, and it needs to be gradually stretched and mobilized by skilled hands. This is not something you can do effectively on your own or with machines.
Act 3: The Thawing Stage (6 to 12+ Months)
Movement slowly starts returning. The shoulder loosens week by week. Without treatment, this stage can drag on for a year or more. With consistent physiotherapy, it can be compressed significantly – sometimes to just 2 to 3 months.
The total natural duration of frozen shoulder without treatment can be anywhere from 12 months to 3 years. With proper frozen shoulder treatment in Indore, many patients regain 80% to 100% of their movement in 3 to 6 months.
The Physiotherapy Playbook for Frozen Shoulder – What Actually Happens in Treatment
If you have been to a clinic where the treatment for your frozen shoulder was an ultrasound machine and a hot pack, you have not received proper physiotherapy. Real treatment for adhesive capsulitis is intensive, hands-on, and follows the stage of your condition precisely.
During the Freezing Stage – Calm the Fire First
When the shoulder is in its most painful phase, the priority is pain management without further irritating the inflamed capsule. Treatment during this stage includes:
- Gentle pendulum exercises – You lean forward slightly and let your arm hang, then gently swing it in small circles. This keeps the joint lubricated without stressing the capsule.
- Pain-free range of motion work – The physiotherapist moves your arm within the range that does not trigger sharp pain, maintaining whatever movement you currently have.
- Soft tissue release around the shoulder – The muscles surrounding the shoulder (trapezius, deltoid, pectorals) often tighten in response to the pain. Releasing this tension reduces overall discomfort.
- Dry needling for trigger points – Painful muscle knots in the rotator cuff and surrounding muscles can be deactivated using thin needles, providing significant relief in many patients.
During the Frozen Stage – Break the Stiffness Systematically
This is where the real skill of the physiotherapist matters most. The shoulder capsule has thickened and contracted, and it needs to be stretched progressively. Treatment includes:
- Joint mobilization techniques – The physiotherapist uses specific graded hand movements (Maitland mobilizations) to gently push the shoulder into greater ranges of motion. These are performed at the precise angle and pressure needed for each patient.
- Capsular stretching – Sustained stretches targeting the tightened capsule in specific directions – forward flexion, external rotation, and internal rotation – where the restriction is greatest.
- Manual therapy combined with movement – Techniques where the physiotherapist mobilizes the joint while you actively try to move in the same direction. This combination produces better results than either technique alone.
- Kinesio taping – Applied to the shoulder to provide support, improve positioning, and reduce pain between sessions.
During the Thawing Stage – Rebuild Strength and Full Function
As range of motion improves, the focus shifts to strengthening the muscles that have weakened during months of disuse:
- Rotator cuff strengthening – The four small muscles that stabilize your shoulder (supraspinatus, infraspinatus, teres minor, subscapularis) need progressive strengthening with resistance bands and light weights.
- Scapular stabilization exercises – The shoulder blade plays a massive role in arm movement. Exercises targeting the muscles that control the scapula restore normal shoulder mechanics.
- Progressive overhead reaching – Gradually reintroducing movements like reaching overhead, behind the back, and across the body that were lost during the frozen stages.
- Functional training – Practicing the actual movements you need for daily life – combing hair, fastening clothes, lifting objects from shelves, driving.
“But My Doctor Said It Will Go Away on Its Own” – The Biggest Myth About Frozen Shoulder
This is technically true. Frozen shoulder is considered a “self-limiting” condition, meaning it does eventually resolve without treatment. But here is what that statement leaves out:
- “Eventually” means 1 to 3 years – That is one to three years of pain, limited movement, disturbed sleep, and inability to perform basic daily tasks. For working professionals in Indore, that means years of compromised productivity and quality of life.
- “Resolve” does not mean full recovery – Studies show that up to 40% of untreated patients are left with some degree of permanent stiffness. They get “better” but never fully regain their original range of motion.
- Diabetic patients often do not self-resolve normally – The glycosylation process that caused the problem in the first place continues if blood sugar is not controlled. Many diabetic patients have prolonged or recurrent frozen shoulder.
- The other shoulder is at risk – Research shows that in over 50% of cases, frozen shoulder eventually develops in the opposite shoulder within 3 to 5 years. Proper treatment of the first shoulder reduces this risk.
Waiting for frozen shoulder to “go away” is like waiting for a rusted door hinge to fix itself. It might eventually move again, but it will never move smoothly unless someone actually addresses the rust.
The Diabetes Connection That Nobody in Indore Is Talking About
If you are diabetic and have developed shoulder stiffness, you need to know something important: your frozen shoulder is not just a shoulder problem. It is a symptom of what uncontrolled blood sugar is doing to the connective tissues throughout your body.
The same glycosylation process that stiffens the shoulder capsule also affects other joints. Diabetic patients frequently develop a condition called “limited joint mobility syndrome” that can affect the hands, wrists, elbows, and spine. Frozen shoulder is often the most noticeable manifestation, but it is rarely the only one.
This means that effective frozen shoulder treatment in Indore for diabetic patients must be two-pronged:
- Aggressive physiotherapy for the shoulder itself – Manual therapy, joint mobilization, stretching, and strengthening as described above.
- Blood sugar optimization – Working with your endocrinologist or diabetologist to bring HbA1c levels under control, because without good glycemic control, the shoulder capsule continues to thicken even while treatment tries to stretch it.
At Dr Manisha Mishra’s clinic, diabetic patients with frozen shoulder receive a treatment plan that accounts for their metabolic condition – including exercise prescriptions that support both shoulder recovery and blood sugar management simultaneously.
4 Exercises You Can Start Today If Your Shoulder Is Getting Stiff
These exercises are safe for most people in the early stages of shoulder stiffness. They will not replace professional treatment, but they can slow down the freezing process and maintain the movement you currently have. Stop any exercise that causes sharp pain.
1. Pendulum Swings
Lean forward with your good hand resting on a table for support. Let your affected arm hang straight down. Gently swing it in small circles – clockwise for 30 seconds, then counter-clockwise for 30 seconds. The key is to let gravity do the work, not your shoulder muscles. Repeat 3 times daily.
2. Towel Stretch (Internal Rotation)
Hold a towel behind your back with both hands – the good arm on top, the affected arm below. Gently pull the towel upward with the good arm, stretching the affected shoulder into internal rotation. Hold for 15 seconds. Repeat 5 times. This targets the specific movement that frozen shoulder restricts most.
3. Finger Wall Walk (Forward Flexion)
Stand facing a wall at arm’s length. Place the fingertips of your affected hand on the wall at waist level. Slowly “walk” your fingers up the wall, raising your arm as high as you comfortably can. Hold for 10 seconds at the top, then slowly walk the fingers back down. Repeat 10 times. Mark the height you reach each day – you should see gradual improvement.
4. Cross-Body Stretch (Horizontal Adduction)
Use your good hand to lift your affected arm at the elbow and bring it across your body toward the opposite shoulder. Apply gentle pressure to stretch the back of the shoulder. Hold for 20 seconds. Repeat 5 times.
These four exercises, done 2 to 3 times daily with consistency, can make a meaningful difference – especially if you are in the early freezing stage. But if your range of motion is already significantly limited, you need professional hands-on treatment to make real progress.
What Sets Dr Manisha’s Frozen Shoulder Treatment Apart in Indore
Frozen shoulder requires patience, precision, and a physiotherapist who understands both the condition and the person. Most clinics in Indore offer the same generic protocol – heat pack, IFT machine, 5 minutes of passive stretching, done. That does not work for adhesive capsulitis.
Here is how treatment at Dr Manisha Physiotherapy Clinic is built differently:
- Stage-specific treatment – The treatment protocol changes based on whether you are in the freezing, frozen, or thawing stage. Aggressive stretching during the freezing stage can make things worse. Gentle treatment during the frozen stage wastes time. The right intensity at the right time matters enormously.
- 45 to 60 minute one-on-one sessions – Frozen shoulder mobilization requires sustained, skilled manual therapy. This cannot be done in a 15-minute slot while managing other patients.
- Dry needling for deep rotator cuff trigger points – The muscles around a frozen shoulder develop painful trigger points from months of compensatory movement. Dry needling addresses these more effectively than any machine can.
- Diabetic-aware treatment planning – For patients with diabetes, exercise intensity, session timing, and home exercise programs are designed with blood sugar management in mind.
- Orthopaedic backup when needed – In the small percentage of cases where conservative treatment is not producing results after 6 months, coordination with Dr Prince Uchadiya ensures timely referral for procedures like manipulation under anaesthesia or arthroscopic capsular release, followed by structured post-surgical rehabilitation.
10 Most Asked Questions About Frozen Shoulder Treatment in Indore
1. How long does frozen shoulder last?
Without treatment, frozen shoulder can last 12 months to 3 years. With consistent physiotherapy, most patients regain functional movement in 3 to 6 months. Diabetic patients may take longer, typically 4 to 8 months with treatment.
2. Can frozen shoulder come back after treatment?
Frozen shoulder rarely recurs in the same shoulder once fully recovered. However, the opposite shoulder develops the condition in about 6% to 17% of cases, and this risk is higher in diabetic patients. Maintaining a regular shoulder exercise routine reduces this risk.
3. Is frozen shoulder more common in women?
Yes. Women are approximately two to four times more likely to develop frozen shoulder than men. The condition is most common in women between ages 40 and 60, particularly those with diabetes or thyroid disorders.
4. Should I get an MRI for frozen shoulder?
Frozen shoulder is primarily diagnosed through physical examination – the characteristic pattern of restricted movement in all directions is usually enough. An MRI is only needed if the doctor suspects a different condition like a rotator cuff tear, which requires different treatment.
5. Will a steroid injection cure my frozen shoulder?
A corticosteroid injection can provide significant pain relief, especially in the early freezing stage, and can make physiotherapy more effective by reducing inflammation. However, the injection alone does not cure the condition. It needs to be combined with physiotherapy for lasting results. Diabetic patients should know that steroid injections can temporarily raise blood sugar levels for a few days.
6. I have diabetes and my shoulder is getting stiff – what should I do first?
Start moving the shoulder gently with the home exercises described above, and book a physiotherapy assessment as soon as possible. Also review your blood sugar control with your diabetologist – uncontrolled HbA1c levels accelerate the capsule thickening. Early intervention in diabetic frozen shoulder produces much better outcomes than waiting.
7. Can I do physiotherapy for frozen shoulder at home?
Home exercises are a critical supplement to clinic treatment, but they cannot replace hands-on manual therapy. Joint mobilization, capsular stretching, and trigger point treatment require the skilled hands of a trained physiotherapist. Think of home exercises as the homework that supports your recovery between professional sessions.
8. Is it normal for frozen shoulder to hurt more at night?
Yes. Night pain is one of the hallmark symptoms of frozen shoulder, particularly during the freezing stage. Lying on the affected side compresses the inflamed capsule, and the shoulder tends to stiffen when held still during sleep. Sleeping with a pillow supporting the affected arm can help. As treatment progresses, night pain is usually one of the first symptoms to improve.
9. How many physiotherapy sessions are needed for frozen shoulder?
Most frozen shoulder patients need 12 to 20 sessions spread over 6 to 12 weeks. The exact number depends on the stage at diagnosis, severity of stiffness, whether diabetes is present, and how consistently you do home exercises. Your physiotherapist will set clear milestones and adjust the plan based on your progress.
10. When does frozen shoulder need surgery?
Surgery is considered when 6 to 9 months of consistent physiotherapy and other conservative treatments have failed to produce meaningful improvement. Surgical options include manipulation under anaesthesia (where the shoulder is forcefully moved while you are asleep to break up adhesions) and arthroscopic capsular release (where the tight capsule is cut through small incisions). Both require intensive post-surgical physiotherapy for full recovery.